Fetal and neonatal alloimmune thrombocytopenia (FNAIT) can occur in pregnancies or post-delivery as a result of a platelet antigen incompatibility between mother and baby. However, the factors involved in predicting the severity of the condition are still being studied.
Recent findings have shown that placental inflammation and disruption could make FNAIT more severe.
What is the role of placental inflammation in FNAIT?
More study needs to be done to better understand the correlation between placental inflammation and FNAIT. However, in a study of placentas in FNAIT-affected pregnancies, placental chronic inflammatory lesions were found in 85% of cases. While it doesn’t trigger FNAIT, placental inflammation is thought to play a role in intensifying the maternal immune response and increasing the severity of symptoms.
The placenta is an organ that connects the fetus to the mother, delivering vital oxygen and nutrients and filtering out waste and carbon dioxide throughout pregnancy. It also acts as the lungs, kidneys and liver of the fetus until delivery and passes on the mother’s immunity to the fetus.
If the placenta becomes damaged or inflamed, it can affect how the placenta functions. In FNAIT-affected pregnancies, it is suggested that placental inflammation can lead to higher rates of antibody transfers via the placenta, accelerating fetal platelet destruction.
What can cause placental inflammation during pregnancy?
Placental inflammation can occur when the maternal immune response is triggered by any of the following:
- Foreign proteins such as incompatible fetal platelet antigens (as in FNAIT)
- Bacterial or viral infections
- Autoimmune disorders
- Emotional or physical stress
- Maternal illness
- Preeclampsia
- Damaged placental development or blood flow
In FNAIT-affected pregnancies, the risk exists when the fetus’s inherited paternal platelet antigen is incompatible with the mother. Following maternal alloimmunization, antibodies cross the placenta to attack the fetal platelets.
It is thought that these maternal antibodies also have the potential to damage placental cells, causing placental inflammation that affects blood flow and could trigger preeclampsia.
How to detect and treat placental inflammation during pregnancy
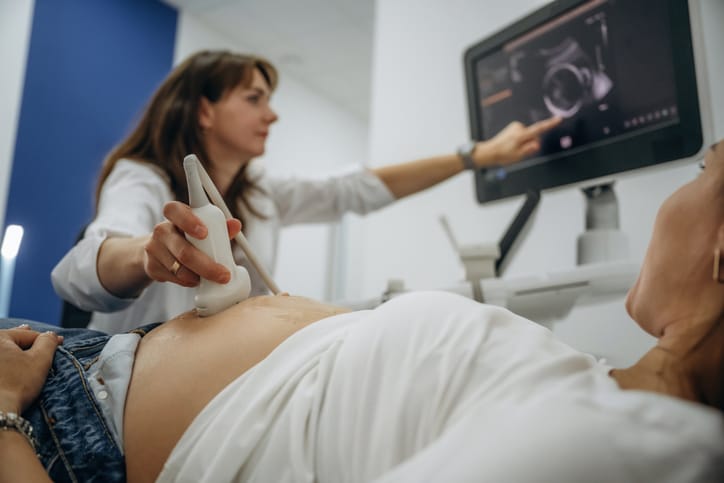
Placental inflammation during pregnancy is not easy to identify and is only detected indirectly through symptoms such as fever, signs of infection, vaginal discharge. It can be diagnosed through blood and urine tests. The functioning of the placenta can be monitored via ultrasound by measuring blood flow, fetal growth, amniotic fluid levels and other abnormalities.
Treating placental inflammation depends on the suspected cause. Antibiotics will be given in the case of infection, and in FNAIT-affected pregnancies, intravenous immunoglobulin is given to help regulate the maternal immune response. Close monitoring and early delivery are also key elements of care when placental inflammation is a possibility.
Sign up here to get the latest news, perspectives, and information about FNAIT sent directly to your inbox. Registration is free and only takes a minute.